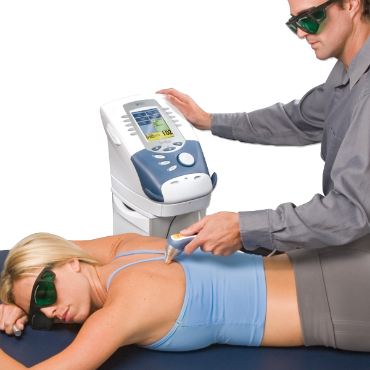
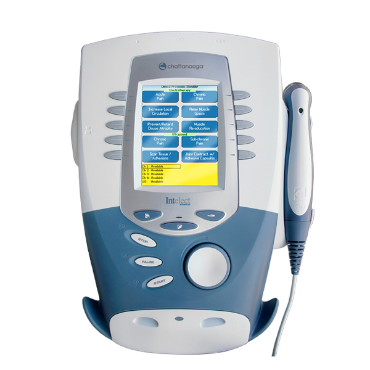
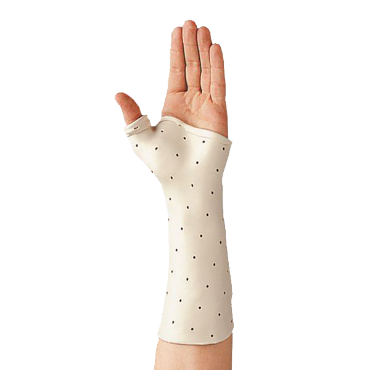
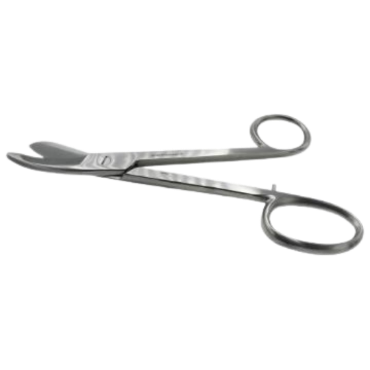
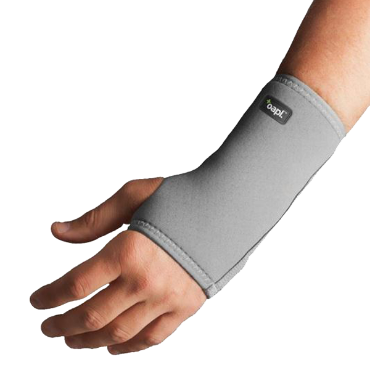
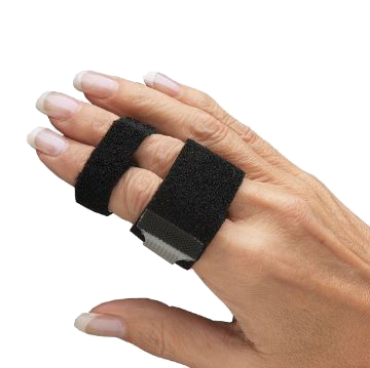
Clinic equipment, practice supplies and treatment tools for Hand Therapy, Physiotherapy, Podiatry, Osteopathy and more.
Compression stockings, sleeves, garments and pumps for the management of Lymphoedema, general swelling, poor circulation and more.
Australia’s largest prosthetic range! Including prosthetic feet, knees, upper limb systems, fabrication supplies and more.
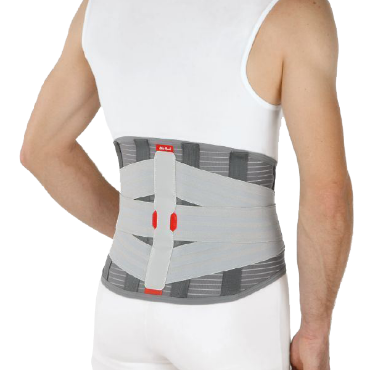
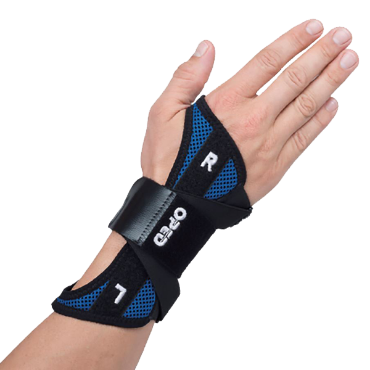
A complete range of bracing from head to toe. For managing acute injuries, post-operative care, neuromuscular conditions and more.